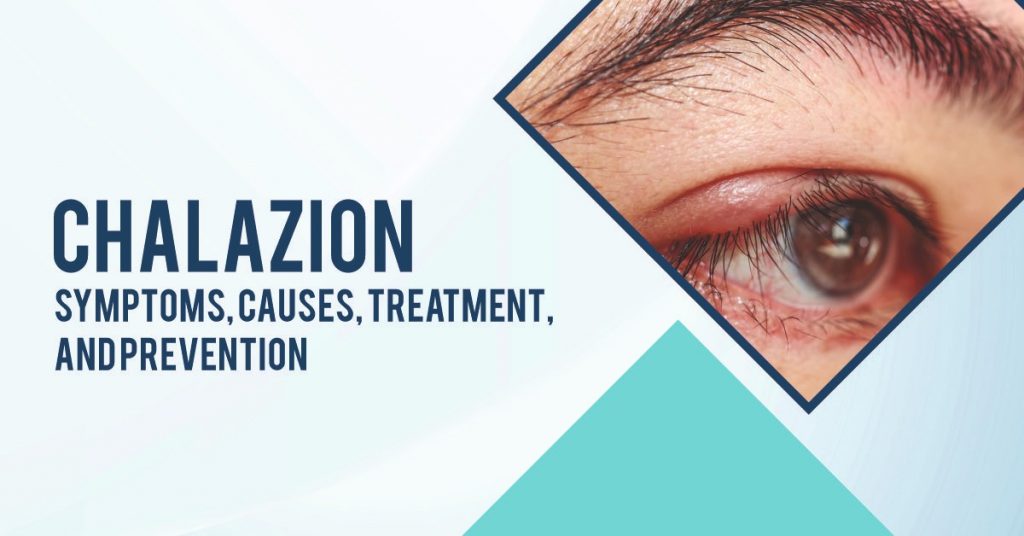
What is a chalazion?
Chalazion (also known as Meibomian cyst) is a cyst in the eyelid caused by a blocked meibomian gland. The cyst is typically in the middle of the eyelid, is red, and is not painful. They usually appear gradually over a few weeks.
A chalazion may occur after a stye or if hardened oils block the gland. Meibomian glands are typically blocked, but Zeis glands can also malfunction.
To keep your eyes moisturized, your eyelids contain tiny glands that secrete an oily substance. Rather than experiencing pain, a chalazion occurs when one of these glands becomes obstructed.
Is chalazion is a stye?
The skin around or inside the eyelids may develop lumps called styes and chalazia. The symptoms may be painful or annoying, but they rarely lead to serious complications. The majority of these will disappear without treatment.
Infections that cause tender red lumps on the eyelids are called styes. Styes are most common along the eyelid edge. It is called an internal hordeolum when a stye occurs inside the eyelid. An external hordeolum appears at the base of the eyelash. Hair follicle infections are the most common cause. You might think it’s a pimple at first glance.
A chalazion is a lump that forms on the eyelids. Although chalazia can look like styes, they are usually larger and don’t hurt.
A bacterial infection is the cause of styes. The bacteria usually grow at the root (follicle) of an eyelash. The infection in a tiny oil gland of the eyelid causes a stye.
During the stye growth, the eyelids may become swollen and painful, and an eyewatering may occur. It normally takes 3 days for the styes to break open and drain. Most styes will heal within about a week.
Causes of Chalazion
The development of chalazia is often caused by something blocking the small oil gland inside the eyelid. Keeping the eyes moist is the function of these glands. Oil starts to accumulate in a blocked gland, which swells. The fluid on your eyelid will drain eventually, so you may have a lump.
The following are some additional causes of chalazia:
- Rosacea (an inflamed skin condition that causes acne and redness).
- Efficacy of topical medications for chronic blepharitis, inflammation of the eyelid (redness, swelling, irritation).
- Seborrheic dermatitis (which is characterized by a red, dry, flaky, itchy face).
- Infectious tuberculosis (TB).
- Infections caused by viruses.
Chalazion Risk Factors
Adults have a higher prevalence of chalazia than children. Your chances to have a chalazion is higher if you have:
- A condition of inflammation of the eyelid (blepharitis)
- It might be seborrheic dermatitis, acne rosacea, or an inflammatory skin condition
- The presence of other diseases, such as diabetes and tuberculosis
- Previous experience with chalazion
What are the symptoms of a chalazion?
In most cases, a chalazion is a harmless lump or swelling on your upper or lower eyelid. In addition to affecting the upper and lower lids, chalazia may also affect both eyes simultaneously. Depending on the size and location of the chalazion, it may cause blurriness or obstruction of vision.
You Can Read Also: What is Cataracts
A chalazion can be red, swollen, and painful if it is infected, although it is not as common. This condition occurs more often in adults than children; most commonly in people between the ages of 30 and 50.
Additionally, you can have:
- An unsightly bump on the upper eyelid that is painless.
- Irritation leading to watering of the eyes.
- The heavy appearance of the eyelids
- A chalazion pushing against the eyeball causes blurred vision.
There is no guarantee that the symptoms described above indicate you have a chalazion. Please consult your ophthalmologist if you experience any or all of these symptoms.
Diagnosis of chalazion
The diagnosis of chalazia cannot be confirmed with a specific test. When you have a chalazion, you will usually seek treatment from an eye specialist. A doctor of optometry or ophthalmology might examine you. In this case, healthcare providers can examine the chalazion and prescribe treatment options.
When you visit an eye specialist, you can expect:
- Please include your full medical history. This data can provide clues to your provider as to what underlying problems might be causing the chalazion to form.
- Your provider is likely to examine your eye, eyelid, eyelashes, and skin texture during an external examination.
- In a thorough eyelid examination, eye specialists use magnification to examine the base of the eyelashes under bright lights. In addition, they examine the openings of oil glands.
Potential Misdiagnosis
In cases where lesions appear around the eye, a chalazion may not be the best diagnosis.
Lesions that appear frequently in the same place, don’t respond to treatment, or are strange in appearance are cases to notify an ophthalmologist. There may be another health issue underlying the lesion.
Among the medical conditions that can lead to misdiagnosis are:
- There is a possibility that these abnormal masses of tissues are benign or malignant. To exclude cancers such as sebaceous gland carcinoma, basal cell carcinoma, squamous cell carcinoma, and Merkel cell carcinoma, a biopsy and microscopic analysis will be required.
- Infectious masses. Meibomian gland drainage can be affected by leishmaniasis or tuberculosis (TB). Eye care specialists may have more insight into the health issue due to the travel history, immune status, and exposure to TB of a patient.
- Immune disorders. In patients suffering from an immunodeficiency disorder such as AIDS or other diseases that affect the immune system, ophthalmic features in hyper-IgE syndrome can occur.
Treatment for Chalazion
Home treatment:
In most cases, chalazion usually resolves on its own within a few weeks without any medical assistance. It may take 2 weeks or 1 month or even 6 months.
During this time, it is best to avoid squeezing or popping the chalazion, as this can increase the possibility of an eye infection.
It is possible to speed up the healing process with several safe ways that promote drainage. The following are among them:
Warm compresses:
A warm compress can be applied to the affected eye to soften any hardened oil blocking the gland ducts. This opens the ducts and improves drainage, which can reduce irritation.
Use and make a warm compress as follows:
- In a bowl of warm water, soak a soft, clean cloth or cotton pad.
- Make sure all excess liquid is wrung out.
- Put the damp cloth or pad on the eyelids and let them sit for 10–15 minutes.
- The compress should be kept warm by frequently wetting it.
- It is recommended to repeat this daily until the swelling is reduced.
Gentle massage:
The oil ducts can be more effectively draining by gently massaging the eyelids each day. If you are going to do this, ensure your hands are clean to reduce the chance of infection. Keeping the area clean and avoiding contact with the chalazion once the draining has begun is crucial.
Surgery:
A doctor may recommend surgery to drain a chalazion if it is severe or persistent. If it is troublesome or persistent, a small operation might be a good idea. For this, your physician can refer you to an eye surgeon (ophthalmologist).
Most of the time, the operation is carried out under local anesthesia, but some patients, particularly children, may need a general anesthetic instead. There is a numbing effect on the eyelid. On the inside of the eyelid, a small cut is made to release the contents of the cyst, then it is scraped out. It is common to prescribe antibiotic drops or ointment after surgery.
Steroid injection:
A soluble steroid injection, generally 0.1 to 0.2 ml of triamcinolone acetonide (TA), may be given intralesionally or subcutaneously to treat chalazia, as the inflammatory cells are sensitive to steroids.
Approximately 77% to 93% of the applications are successful. There is the possibility of occlusion of the central retinal artery, acne-related focal depigmentation, and inadvertent ocular penetration in dark-skinned patients.
You Can Read Also: BAD BREATH: CAUSES, TREATMENTS, AND PREVENTION
Among the many treatment options available, it’s simple and effective, with a high success rate. It may achieve the same results as orthopedic surgery (I&C). Surgical treatment is recommended for lesions that have been present for a long time.
For marginal lesions and those located near the lacrimal punctum, steroid injections are preferred over surgery because of the risks of surgery. Injections alone have an 80% success rate. If needed, a second injection can be administered approximately one to two weeks later.
Carbon dioxide laser:
Using a CO2 laser for chalazion excision is also a safer procedure with minimal bleeding and no need for eye patches
Over-the-counter treatments:
A chalazion or stye can be treated with many over-the-counter products. By reducing irritation and preventing infection, these remedies may speed up healing. Medicated eye pads, ointments, and solutions are some of these products. It is beneficial to get advice from a pharmacist.
Complications during chalazion:
When the cornea is compressed, astigmatism can result from a large chalazion.
Due to the use of lasers for corneal surgery, where parts are burned away, leaving the cornea weak and vulnerable, people can develop deformities in the cornea after the operation from small chalazion.
The conjunctival approach of injection, however, is less likely to result in adverse effects such as hypopigmentation and fat atrophy.
Occasionally, chalazion recurrence at the same site may indicate sebaceous cell cancer
Prevention of chalazion
If you follow good hygiene habits, you can avoid getting chalazion. The following are essential elements of good hygiene:
- Hand-washing: Wash your hands frequently and thoroughly. Touching your eyes should be done only after washing your hands.
- Contact lens care: Before removing your contact lenses, wash your hands. Ensure that your contacts have been cleaned thoroughly with a disinfectant and lens cleaning solution. Don’t forget to throw away daily and limited-time contacts on time.
- Face-washing: Remove dirt and makeup from your face by washing it every day. For people with blepharitis, a special scrub or baby shampoo may be recommended to cleanse your eyelids.
- Makeup hygiene: You should throw away all of your old makeup. Every two to three months, be sure to replace your mascara and eye shadow. Be careful about sharing and using other people’s makeup.
- Warm water compression: Using a warm compress on closed eyelids three times a day for five minutes before sleep can help prevent the Meibomian gland from clogging in the middle of the night.
- Gentle massage: Do a gentle massage over and under your eyelids every day for two to three minutes. You can use this method to unclog your oil glands.
How long will I have a chalazion?
There will be differences in the results from patient to patient and from condition to condition. Generally, a chalazion can last for a week, a month, or even longer. Chalazia is more common among patients with blepharitis, an inflammation of the eyelids.
Rub one’s eyes frequently and have poor hygiene, and you are more likely to get styes and chalazia. The children can also pick at them, causing simultaneous cellulitis, even though they are not dangerous. In the absence of oral antibiotics, cellulitis can be fatal.
In most cases, a chalazion will heal within one week, or less, if treated properly.
Conclusion:
First, everyone thinks it’s a pimple near the eyelid, but it’s usually not. You may have a stye or chalazion. However, if it is not causing pain, it is most likely a Chalazion. There is no acute or fatal infectious disease associated with a chalazion. This type of skin condition can occur to any person who is careless when it comes to their skin and face.
Preventative measures are better than cures, as we all know. Make a habit of washing your face every single day at appropriate intervals of time, ensuring good hygiene.
Within one month or six months, the disease will be cured. A chalazion is a self-cure disease that will go away without treatment but if it does not go, you should take the proper advice of your doctor and be regular with the treatment.
Several treatments are available, including water compression, gentle massage, maintaining proper hygiene, small surgeries, steroid injections, and antibiotic creams.
Don’t neglect your skin and health. Maintaining good hygiene and drinking a lot of water are the keys to healthy skin.